The Alternative option: Soft-Cuffs (Emergency Response Cuff – ERC)
An innovative and very significant restraint device is now available to hospitals and care services in the UK and we believe that it deserves a serious and comprehensive exploration.
The equipment is formally known as the Emergency Response Cuff (ERC) and is sometimes referred to as the “Soft-Cuff” due its tough-cloth construction. While sharing many characteristics with its long-standing law-enforcement cousin, the metal handcuff, some could say that this new device is an important evolution on a theme.
This restraint equipment has recently been released to healthcare and police services, following an expert medical review and the development of a comprehensive training programme for its use in a variety of settings where it is gaining much attention and some popularity.
I recently had the opportunity to spend a significant amount of time becoming familiar with, using and observing the training of teams who are adopting the Emergency Response Cuff (ERC) and I thought that my experiences might be useful to managers, trainers and teams who are interested in this new development.
The Product
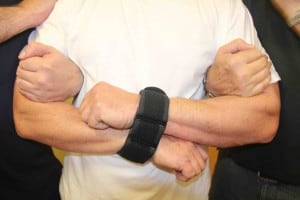
The ERC has two lengths of universal velcro, bound and sewn together at one end where a pair of D-rings allow the tips of the lengths of velcro (the compression straps) to loop around and form circular enclosures.
To the touch, the fabric of the ERC gives the impression of being extremely tough but also surprisingly flexible and indeed soft to the touch. This pliability of the material becomes important when applying the ERC to a subject – the ease with which the staff can turn and flip the material assists easy application.
The current model of ERC incorporates a new D-ring design, introduced in order to make sure that insertion and extraction of the compression straps could be as simple as possible for staff. The manufacturer has also uprated the strength of the D-ring to the highest level.
One important point to note is the relative comfort of being held in this device. On the numerous occasions when the ERC was applied to me during training it did not leave marks, although applied with enough security to leave me under firm control. This is a key differentiator when considering the alternatives to ERC – various kinds of metal cuff (rigid, hinged or chain).
BENEFITS OVER TRADITIONAL RESTRAINTS
Whereas metal cuffs almost always leave marks and reddening (and I am aware of the potential civil claims which can result from that in my role as an expert witness), I found that the soft-cuffs were not as likely to do so.
This benefit – comfort and safety – appeared as one of the main beneficial features mentioned by the staff teams I was encountering. Here was a potential, viable alternative to metal cuffs for their clients in severe learning disability and mental health settings.
Some teams are substituting Soft-Cuffs for this purpose, increasing the level of comfort for the patient while also removing or reducing the ‘police case’ stigma that attends the use of metal cuffs. I overheard one team who were evaluating the Soft-Cuffs saying “this [soft cuff] feels more like something I would use in a healthcare environment” rather than metal cuffs, for example.
LONG-STANDING AND SAFE PEDIGREE
The ERC is part of a product family which started with the Emergency Response Belt (ERB) which is a restraint device from the the USA and which has a very successful history. The ERB has been in use by emergency responders of all kinds to assist in the control of violent subjects for almost two decades in the UK, having first been adopted by police agencies looking for ways to control people involved in, for example, acute behavioural disturbances.
The safety record for ERB is remarkable in that there have been no adverse incidents due to its use. One of the reasons for this is that the equipment itself is only released to individuals, teams or organisations who have had accredited training in the safe and appropriate use of the device.
It is therefore worth noting that any organisation or team who want to procure the ERB or ERC devices would first have to evidence that they have had full, accredited training from a competent ERB/ERC trainer before the equipment will be shipped to them.
Training is accompanied by a full manual, including advice on the storage and care of the device as well as comprehensive instructional details on the safe and appropriate application of the device for different needs.
In the next part of this blog, I want to explore some of the scenarios in which teams are examining the ERC Soft-Cuff and ERB Response Belt.
Scenarios for the use of the ERC Soft-Cuff
Having introduced the Emergency Response Cuff and explained something about its shape and function, I want now to explore the scenarios in which staff might consider the use of the ERC.
First we should cover the rights and responsibilities of staff which give them the power to use force. The right to make physical interventions is enshrined in law and guidance, for example:
- The Common Law
- The Mental Health Act
- The Mental Health Act Code of Practice
- The NICE Guidance on the Short-Term management of Violent Behaviour
- The Mental Capacity Act
The overarching principle or ‘golden thread’ which runs through these acts and guidance in care is that an intervention which limits the freedom of an at-risk person should be the “least restrictive option” available which achieves the legitimate aim being pursued.
In the Mental Health Act Code of Practice there are guiding principles:
15.9 Any such intervention must be used in a way that minimises any risk to the patient’s health and safety and that causes the minimum interference to their privacy and dignity, while being consistent with the need to protect the patient and other people.
15.11 Patients who are identified as being at risk of disturbed or violent behaviour should be given the opportunity to have their views and wishes recorded, in the form of
an advance statement. They should be encouraged to identify as clearly as possible what interventions they would and would not wish to be used.15.12 dignity. These are essential values that must be engendered and asserted
in all policy, educational material, training, and practice initiatives related to the safe and therapeutic management of patients.15.22 Any physical restraint used should: be used for only as long as is absolutely necessary;
In my experience of training teams in the use of the ERC, staff have been very keen to weigh and consider the appropriateness and effectiveness of the device in varied scenarios they see in their environments.
For example trainers have considered that ERC may assist staff with:
A) Reducing Risk during Transport
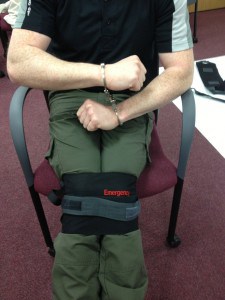
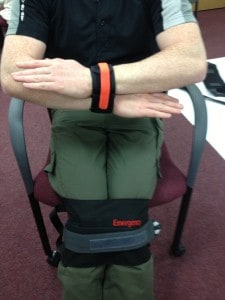
Staff have considered the use of the ERC in safely transporting service users from area to area or from secure settings to non-secure settings, using the device as an alternative to handcuffs made of metal.
The Soft-Cuff can be used as an alternative for traditional metal cuffs. For example, at the moment in many NHS trusts metal cuffs are used when transporting patients from secure areas to appointments in other less-secure hospital settings. Currently, metal cuffs are often applied to the patient with the patient’s consent and the method of application is to the front of the person in a palm-to-palm method.
In addition to this, teams often take steps to protect the dignity of service users by making the presence of a restraint device more difficult to see, for example when a patient is in a public area. Staff will sometimes use a sweatchirt or cardigan folded over a restraint device in order to make sure that it is as unobtrusive as possible.
B) Reducing Risk of Serious Self-Harm
Staff have considered the use of the ERC Soft-Cuff in effectively safeguarding service users who present a known risk of significant self-harm.
Many parts of the NHS look after extremely vulnerable people with learning disabilities or mental illnesses. A proportion of those vulnerable people in care exhibit exceptional self-harming behaviours.
Those behaviours include for example:
- constantly putting their fingers down their throat to induce vomitting
- striking their head against a wall at full force to deal with frustration
- pulling hair and peeling skin from their body to reveal underlying bones and tissue
At times these behaviours can be life-threatening or at the very least can present the risk of causing serious deterioration in the person’s quality of life or their health and safety. It then becomes incumbent on the nurses and carers to make an intervention – if it is absolutely necessary and in that person’s best interest – to stop that harm from occurring.
In many cases, staff will legitimately use physical restraint interventions to stop or minimise the harmful consequences of these behaviours. A team will employ a physical holding method to immobilise the person concerned in a way which makes it difficult or impossible for them to continue injuring themselves.
One issue which arises from this is that there are incidences where a team must continue to hold the person for long periods of time. This sometimes extends to many minutes, or even hours, extending into full shifts where staff will be employing a tag-team approach and swapping tiring team-members for fresh ones to maintain control of the person. I will explore this issue more deeply in a following post.
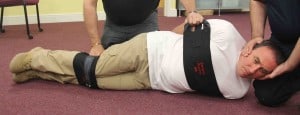
C) Reducing Risk during Emergency Restraint / Minimising Prone Restraint
During an incident where a patient becomes extremely agitated and violent, perhaps attacking another patient or attacking a member of staff, it is necessary to restrain the patient. These ‘emergency restraint’ interventiosn can be extremely chaotic and violent. Violent struggles during restraint often mean that the restraint will end up on the floor.
Staff in healthcare accross the UK are routinely trained in how to restrain a patient on the floor – often face-down in the ‘prone position’ – in order to gain the greatest safe control of the person in exceptionally dangerous circumstances.
The focus of much controversy and conflicting opinions, the relative safety of restraint in the prone position attracts much attention. Prone restraint has been associated with sudden deaths of people in care. This association between prone restraint and sudden deaths is constantly under examination and remains a controversial but strong association rather than a definite and recognised cause. For good reason, training programmes and policies tend to seek to limit the use of prone restraint to situations where it is an absolute last resort.
There are situations where staff have had to bring a person under control in the prone position, so we must then ask: “Prone position, and thenwhat?”
If prone restraint is the last option, staff may have nowhere else to “go” once they have established physical control on the floor.
In some settings, the staff will be authorised to use chemical control or rapid tranquilisation to influence the patient’s behaviour and this is often administered to the patient when they are prone.
However, sometimes the standard medications used for this purpose to not have the desired effect on the patient, or do not have the desired effect soon enough to control the risk. The length of time it takes for rapid tranquilisation to take effect is often measured in terms of minutes, not seconds.
The more powerful the tranquilising medication, the greater the side-effects and potential health problems which may result, further complicating the control of risk in the scenario.
Given this type of scenario, it is appropriate for managers, trainers and staff to ask: “If we could use a restraint device to reduce the risk more quickly and comfortably – should we?”
In the next part of this blog, I want to explore how the ERC (and its older cousin the ERB) may reduce risk for all concerned by bringing situations under more control more quickly and comfortably.
NEXT: How do Restraint Devices such as the ERC positively reduce risk?
How do Restraint Devices like ERB and ERC “Soft Cuff” address risk positively?
We have looked at how there are a number of scenarios in which staff are faced with difficult decisions about how they can maintain care and control of their patients and clients, while being aware of the the risks involved. Some staff, as we have seen, are exploring ways of using restraint devices such as the Emergency Response Belt (ERB) and Emergency Response Cuff (ERC) to control those risks in the best interests of the client.
We mentioned the risks from traditional metal cuffs, from prolonged manual restraint and from the reliance on prone restraint or medication to subdue violent clients. I want to delve a little deeper into those risks now so that we can be clear on why a team might choose to use the ERB or ERC.
Some of the issues involved are what are the Employer’s duty of care obligations as follows:
- the manual handling issues when staff engage in prolonged manual restraint of patients?
- the medical and psychological considerations for the patient in prolonged manual restraint?
- care planning issues for the patient who is subject to long periods of manual restraint?
- the risks attendant to the use of traditional metal cuffs?
Employers are responsible under Management of Health & Safety at Work Regulations 1999 to carry out risk assesssments, so it becomes important to question the risks to everyone involved, both physical and psychological, when higher-risk interventions are required in the client’s best interests.
Issue 1: Subject Fatigue
The tragic death of Anthony Pinder in a care home in Grimsby in 2004 serves to underline the risk of prolonged restraint:
Forty-two year-old Anthony Pinder, who had learning and behavioral issues, was physically restrained for around 90 minutes by staff at the Old Vicarage nursing home in Stallingborough, near Grimsby, on 1 October 2004. He was eventually released and crawled unaided to his room, but was found dead a short time later.
Prolonged physical restraint is exhausting for the subject – whether their mental state will allow them to be aware of it or not. In fact, in Police Complaints Authority guidance issued in 2002, entitled “Policing Acute Behavioural Disturbance”, the advice is as follows:
The amount of time that restraint is applied is as important as the form of restraint and the position of the detainee. Prolonged restraint and prolonged struggling will result in exhaustion, possible without subjective awareness of this, which can result in sudden death.If possible, avoid the situations in which prolonged restraint and prolonged struggling, become necessary. If the person has to be restrained, avoid pressing down on the trunk. Use the limbs. Binding the ankles wand wrists will be considerably safer than kneeling on the back of someone’s chest.
The combination of fatigue, prolonged struggling, physiological arousal, respiratory distress followed by cardiac arrythmia and arrest is an all too common deadly mix seen in restraint-related sudden deaths.
Violently struggling against a team of staff who are holding the client for significant time periods is an identified risk-factor in these cases.
Is it possible that the use of a restraint device would significantly cut the amount of time during which the person would be struggling in a vulnerable position?
Issue 2: Staff Fatigue
We have explored subject fatigue and the position of the subject as complicating factors in safeguarding during physical interventions, however there is one more reason why a restraint device should be considered within the range of options – staff fatigue.
In fact, in the tragic case of the restraint-related death of Geoffrey Hodgkins, there is the suggestion that staff were ‘swapping out’ due to fatigue during the long period of time in which restraints were going on with him. Prolonged restraint is known to increase the risk of sudden death for the subject, however it is often overlooked that the staff in our services are also vulnerable to the effects of sustained physical exertion.
It can be, for some administrators, difficult to imagine the sheer physical exertion which is necessary when frontline staff successfully carry out a restraint intervention. For example, there is at least one instance that I am aware of whereby a member of a restraint team suffered a heart-attack while involved in the prone restraint of a violently struggling subject.
There exists a phenomenon in personal safety training which is called the Fatigue Threshold – “the sudden physical exhaustion experienced during a force encounter when an [staff member] cannot effectively perform to either control a [person] or defend himself.” This threshold can be reached within as little as 30 seconds or in the case of a very physically well-conditioned staff member, just 5 minutes.
The practitioner who researched this phenomenon and coined this term states that
“The closer an officer gets to his or her personal fatigue threshold, the more dangerous the situation becomes, not only to the officer, but often to the subject as well. You’ll do anything to avoid it, including using what may otherwise be considered excessive force.”
“Don’t figure on most people being able to hold out for more than 2 minutes or so,” he advises. “You don’t have much time to get a subject under control before you’re going to be in trouble.”
Is it possible that by having a secure way to restrain the subject – which uses the mechanical advantage of velcro straps rather than muscular exertion – would reduce the risk of reaching the fatigue threshold?
Issue 3: Prone Position and then what?
The prone position remains a highly controversial subject, as evidenced by the recent storm created when MIND released the results of the Freedom of Information study about the Prone restraint of people in mental health care.
Importantly, it is recognised that staff who are struggling to restrain a particularly violent individual will often end up on the floor as confirmed in the 2002 PCA guidance:
If the person has a knife of gun, taking them down to the prone position may be absolutely necessary. However, “the prone position should be avoided if at all possible, and the period that someone is restrained in the prone position needs to be minimised.”
In addition, the chairman of ACPO’s Self-Defence, Arrest and Control Working Group has said in 2013:
“The initial control and restraint of violent individuals is usually a fluid and dynamic process, which often ends up on the floor. The reasons for this are twofold. Firstly, gravity will of course prevail in fast moving incidents where one’s balance is often lost. Secondly, the floor is often the safest place (for all) to achieve control and subsequent restraint of a violent person”.
The issue we have in healthcare, which distinguishes it significantly from the use of force by police, is that the police will use the prone position in order to secure the individual in a set of handcuffs and other restraining devices. Healthcare staff do not typically have this final step in a Control & Restraint process.
In some healthcare environments, there is a possible resort to chemical restraint, however this option comes with its own significant limitations. The application of rapid tranquilisation can:
- take a significant amount of time (see fatigue threshold above) measured in minutes not seconds
- sometimes not have any or enough effect on the person’s behaviour
- if delivered in enough amounts to have a significant effect on the person, can subsequently put their life in danger.
Healthcare staff are therefore left with some less-desirable options:
- continue to hold the person down until they become calm / weak / unresponsive
- let the person up out of the prone hold but sacrificing the control which necessitated it
- use Rapid Tranquilisation which may or may not work in time to control the risk
The report into the tragic case of the death of psychiatric patient Geoffrey Hodgkins, who died in 2004 after being restrained on the floor in the prone position for over 25 minutes while waiting for medication to take effect, is a sobering example of this forseeable scenario.
Is it possible that SoftCuff and ERB devices could offer healthcare staff a safer ‘next step’ to move towards, once some control has been achieved in prone restraint?
NEXT: let’s look at three criteria which are often applied to any analysis of the suitability of a restraint procedure – Manual Handling, Duty of Care and the Best Interests of the client.
Applying Manual Handling criteria
The physical handling of any load or person is regulated under the Manual Handling Regulations 1992.
The Regulations and Associated Guidance paragraphs establish a clear hierarchy of measures:
1: Avoid hazardous manual handling operations so far as is reasonably practicable. This may be done by redesigning the task to avoid moving the load or by automating or mechanising the process.
2: Make a suitable and sufficient assessment of any hazardous manual handling operations that cannot be avoided.
3: Reduce the risk of injury from those operations so far as is reasonably practicable. Particular consideration should be given to the provision of mechanical assistance. Where this is not reasonably practicable then other improvements to the task, the load and the working environment should be explored.
The Manual Handling Regulations require that any physical intervention procedure staff are using to carry out a task should be assessed in such a way as to reduce forseeable risk.
It seems sensible that the use of a device to assist a hazardous manual handling procedure be considered in the ‘range of options’ available to the staff. Of course, staff already use a device to assist in another hazardous manual handling activity all the time – the hoist!
If a hoist is considered essential for the manual handling of a person who requires lifting, why then would the use of a device to hold them during a violent episode be considered ‘inhumane or degrading’? Particularly when one considers that the use of a device can be in the ‘best interests’ of the person being restrained because it may:
- reduce the time during which staff struggle to gain control
- reduce the amount of time the person is restrained for
- reduce the overall amount of time which the actual task (e.g. personal care) takes
The ERC and the ERB, when used in conjunction with one another, can make the movement or handling of a violently resisting person much safer because of the effect of putting ‘handles on the body’ for moving & handling procedures.
Applying the ‘Duty of Care to Staff’ criteria
Some will be concerned that the use of restraint devices is against their caring ethos. They see the use of devices to restrain as somehow a ‘step backwards’ in terms of care, or somehow intimidating or degrading for the person concerned. Perhaps managers are even afraid that a care inspector might see them using a restraint device and decide that it is ‘abuse’.
There is a case which came to my notice early in 2013 which illustrates how the courts treat the difference between the legal obligations of employers/managers and the ‘caring ethos’ which sometimes clouds decision-making in the care sector.
The case was of a young woman who was working for Bradford NHS trust and who almost lost her sight because of the violent spitting behaviour of her client. Known to spit when frustrated and aggressive, he spat in her face one day, which resulted in an eye infection and necessitated an eye operation to save her sight.
In the court case which ensued, her union and the prosecution lawyers successfully argued that there was no adequate system in place for recognising the risks staff faced with that service user and how best to control those risks. It was specifically mentioned that the staff should have been provided with protective equipment (eye goggles ) to deal with the risk.
It takes little imagination to guess at the reason why management had NOT considered the use of the goggles or spit-masks. In fact I have been involved in meetings where management and staff have discussed the use of a variety of protective equipments to stop staff from being spat at or bitten. Always the issue arises: “would that be a dignified or humane way to treat the service user, in line with our caring ethos?”.
This case severs to remind us all that a decision not to use an ‘obvious’ risk-control method may need to be defended in court if a situation results in harm, injury or death.
To return to the main thread of our discussion here then, my advice is that managers should be:
- actively making themselves aware of risk-control methods which are available in their sector
- assessing the risks facing their staff in an objective way
- considering the use of risk-control methods while considering their legal obligations to BOTH staff and clients
- objectively documenting the reasons why they have decided to use or not use those methods.
My caution here: the choice NOT to use an available risk-control method would need to be carefully, objectively documented in a suitable and sufficient risk assessment.
Applying the ‘Best Interests’ criteria
I often hear that a care home has a resident for whom it becomes necessary to carry out personal care when they are in bed AND they are resistant to that care.
My recommendation has always been that cleaning or caring for an actively resisting mobile person in a bed will require 5 staff. My best example of this is the case of a client in a private hospital I work with who sometimes suffers life-threatening respiratory distress, but who violently attacks the staff who attend to him to save his life.
The procedure we teach staff for this task requires 4 staff to engage and hold the subject and then 1 staff is able to safely carry out the personal hygiene care task. In my opinion, with a mobile person who can move their limbs freely, this is the minimum requirement to carry out the task safely.
One consideration here is that a team of 5 staff with a good plan can complete a cleaning task like this in less time with more safety and comfort for the person than a team of 2 staff can with less control and less safety. A team of 5 staff can complete the task faster by far than a struggling team of 2.
Staff often resist the idea that this task might need so many people, however if we ask the question: what is in the resident’s best interests? then I think the answer would be: “To be subjected to any invasive procedure for the minimal amount of time necessary”
Is it possible that the least intrusive response to a person’s presented behaviour may be the use of a restraint device like Soft-Cuffs or ERB?
In summary then, I believe that the ERB and ERC can serve a very useful purpose for healthcare staff who are facing particularly difficult decisions about how to maintain appropriate care of vulnerable people and at the same apply the right level of control in regard to the risks they face when those clients are violent or combative.
From the point of view of staff, clients and management, these devices should be considered carefully in the light of all the information, guidance and legalities which attend to this complex area. However, complex as it is, I believe that there are situations in which these devices can make the care of vulnerable people both safer and more suited to individuals’ needs.
INVOLVEMENT:
I have one final example of how these devices could be both appropriate and highly useful. I recall hearing that at one NHS trust, a client who has recurring episodes of violence which necessaitate staff having to control him in prolonged holding, the staff asked him about these devices. They involved him in a presentation and demonstration of the devices use, and asked for his opinion as to how they might be used to better deal with his episodes of violence. I think it is a great example of a staff team not just being satisfied with the status quo, and also actively looking for a better way, in cooperation with their client. Bravo!
Gerard O’Dea is a conflict management, personal safety and physical interventions training consultant. He is the training director for Dynamis, a specialist provider of personal safety and violence management programmes and the European Adviser for ‘Verbal Defense and Influence’, a global programme which addresses the spectrum of human conflict. www.dynamis.training




Comments are closed.