Splish, Splash, Splosh – I just got Boshed!
Care assistants and caregivers consistently find that bathing is one of those flashpoints that they have in terms of conflict and combative behavior with elderly residents in care, particularly those who may be confused or distressed because of the effects of dementia.
This is one of the times that we, as a company who teach physical intervention, get called in to talk about how the staff can manage these situations. BUT the first thing we need to talk about is why the client or the resident is becoming stressful at these times?
The vast majority of the work that’s been done on this was done by a number of nursing professionals in the US who studied for well over a decade the various approaches that care assistants and caregivers have to successfully giving personal hygiene and skin care to older people in care, perhaps in situations where those people are becoming distressed.
“Bathing without a Battle” is available on Amazon and other good book stores online (see the link at the end of this article). You could go ahead and get one for your training library, and I would highly recommend that, but right now, I’m going to just go through a couple of the key ideas that that book postulates and see if we can stimulate some conversation through that.

What do you mean, WASH ? ! ? !
One of the really interesting things that this program goes into is our thoughts about what being clean really means and what bathing has meant to people down through the ages.
For example, this image of a woman who’s giving her young child a bath inside the sink, it’s probably in the bathroom of their house, but it’s the most convenient and easy way for her to get the child clean, so there you go. There she is.
Of course, we know that for many, many years, the way that people became clean and got themselves clean was they used a big steel tub in the front room with the fire lit, and they had one amount of water poured in there and that was a ‘communal bathing experience’, so everybody shared the water! This was how most people from decades ago would have had their experience of getting clean.
It might not have been that pleasant, but perhaps that’s part of the key issue here is that we all have different experiences of what bathing means. For some of us it’s positive, and for some of it’s negative, and for some of us, we’ve never had a shower before, or our preferred method of getting clean is just with a soapy face cloth in front of the sink. That’s one of the key issues is to try and change some of the perceptions around what does clean mean, and what is the most effective way to get somebody clean, and we have to talk about those things.
We spend time in our safe caring courses talking to the staff and exploring with them what their bathing environments look like, feel like, and sound like, and we elicit some great suggestions from the staff about how they can start to improve those environments to make them more attractive. The idea here is that when an older person is asked to go to a bath, they perceive it as a spa-like experience and not as some kind of negative or aversive type of experience that they really wouldn’t want to get involved with.
Interestingly, one of the key discoveries that the team working on Bathing Without a Battle found was that a covered, in-bed massage bath was one of the easiest ways that the caregivers described to get their residents clean, and it also was reported as one of the ways that tended to keep their residents more relaxed and more cooperative during the cleaning and the washing experience. So that’s something called a covered, in-bed massage bath, which is detailed with great amounts of information in that book, Bathing Without a Battle, and I believe they even have a DVD that demonstrates the method for those who want to go ahead and explore that further.
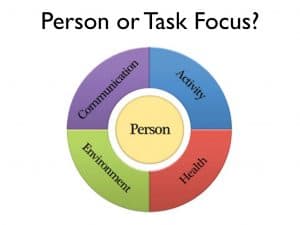
COMMUNICATION
Engaged communication is so important here as well. One of the key flashpoint moments is at the very, very beginning of this process, at the invitation to the bath. How carefully staff can approach the resident and introduce the idea that it’s time for them to go and be clean, is a really key moment. Something that we discuss with a lot of our care staff is that initial greeting and that initial broaching of the subject, and whether or not that person feels that they can connect on a human level with the person who’s asking them this.
INITIAL CONTACT
You might have seen a program in the NHS called Hello My Name Is, which was initiated by a doctor called Kate Granger, who herself was a terminally ill cancer patient. Her point was that if we (care givers, clinical professionals) would just do the basic things about introducing ourselves correctly and matching the pace of our activity with our residents and patients, that perhaps we’ll get better results and would achieve more compassionate care. Certainly, at the beginning of the bathing process, we really need to have that established.
At the complete opposite end of that, and in contrast to it, is what was described as non-engaged communication. That’s when care staff are perhaps just talking amongst themselves, not really engaging with the client about her needs or her wants, and seem to be quite distant although doing something quite intimate with the patient. Of course, this increases stress and probably results in some level of resistance or combativeness.
RIGID POLICIES
We’ve seen ourselves in some care services that we’ve visited the rigid policies that are in place which sometimes make it difficult for individual carers and teams of carers to come up with person-directed plans for bathing with particular residents. Some care homes will have strict plans and directives about bathing or showering, for example the days of the week when that happens, or the times in the day when that happens. Only when we start to become more flexible with these schedules and really try to apply person-directed ideas, principles, to this bathing task, then that’s when we’re going to start seeing a reduction in those battles that happen around bathing time.

THREE AREAS
Interestingly, the research seems to point to three different areas of focus where we can gain a lot of insight into why we have patients and residents who are being resistant at bath time. Those three things were pain, cold, and fear. The suggestion is that if we can focus on identifying the causes of pain, the sources of cold and changes in temperature during bathing, and then try to identify what is it that’s perhaps causing some fear in our residents, and if we can focus on those three key areas, we should see a reduction in the level of combativeness and resistance at that invitation to the bath.
The key tips that came out of the research were things about covering the residents comprehensively, washing single areas at a time and then moving on, timing the bath and choosing the right moment to do it, and, of course, that key idea about matching pace and moving slowly.
For information about our Train-the-Trainer Courses in Conflict Management, Non-Escalation, De-Escalation and Crisis Intervention with our content partner Vistelar, please visit the webpage: www.dynamis.training/vistelar
Please visit www.dynamis.training/safe-caring for details of our entry-level courses in personal safety for care-givers, care assistants, nurses and allied professionals who may need to work in close proximity with unpredictable elderly or other vulnerable client groups. More robust options are taught on our course for safe holding in elderly care (www.dynamis.training/safe-holding) where last-resort, protective interventions may become necessary in higher-risk scenarios.
- Care Home Owner-Operators
- Local Authority Care Home Managers
- Teams of Care Assistants, Nurses and Supervisors
- Social Work Teams who are responsible for High-Risk Service Users with Dementia
This training will enable your teams who look after these residents and patients to understand and empathise with the stress-related behaviours of people who are living with Dementia and to manage them by combining relevant reduced-stimulation approaches, personal safety habits and last-resort physical, protective interventions if they are the appropriate actions to take. Your learners won’t experience a tick-box off-the-shelf training package but instead a properly tailored workshop-type immersive intervention which will take into account their experiences with your clients, specific to the most challenging moments they have with them.
Bathing without a Battle on Amazon: http://amzn.eu/dq15iCY